What Is Hidradenitis Suppurativa?
Reviewed by: HU Medical Review Board | Last reviewed: December 2020 | Last updated: April 2024
Hidradenitis suppurativa, or HS, is a chronic inflammatory skin disease with serious effects on quality of life. It is pronounced HI-drad-en-I-tis sup-per-ah-TEE-vah.1,2
The name comes from Greek (hidros, sweat; aden, gland; -itis, inflammation) and Latin (suppurare, to form or discharge pus). The disease was named officially in 1854 by a French doctor. He thought that inflammation of the sweat glands caused pus and scarring. Doctors now think that HS comes from problems with hair follicles, which are near sweat glands.3-5
What are the symptoms of hidradenitis suppurativa?
Formerly called acne inversa, HS begins with small bumps, like pimples. They are mostly found:1,2,6
- In the armpits
- In the groin
- Under the breasts
- On the buttocks
- In the anal and genital areas
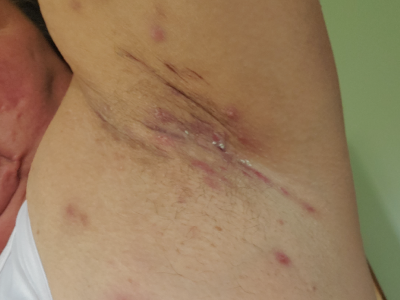
Itchy or painful bumps return again and again when the disease flares. HS can lead to painful abscesses and sinus tracts, which are narrow tunnels extending under the skin from a wound. A discharge of pus and an odor often make HS discomfort worse. After healing, wounds can leave scars.1,2,6
Who gets it?
The exact number of people with HS is not known. Doctors believe as many as 4 out of every 100 people in the United States have HS. HS can develop at any age, but it is most common for people to develop symptoms when they are between the ages of 30 and 40. HS is more frequent in women, and people who are Black or biracial (Black and white).7,8
What causes it?
HS begins with blockage of a hair follicle, the tiny canal in the skin where a hair grows. Clogged follicles cause bumps, like pimples. Eventually, the follicles burst and cause odor and discharge. The immune system then triggers an inflammatory response. Bacteria may cause an infection that makes HS worse.9
As the disease worsens, the process repeats again and again. It causes sinus tracts connecting the lesions, or sores, to form. The wounds usually leave scars when they heal.9
About 35 to 40 percent of people with HS have a family member who also has it. This suggests that genetics might be a factor. Researchers believe that more than one gene is involved. A mix of factors can contribute to HS, including:2,6,10
- Friction from clothes and body folds
- Heat and sweat
- Hormones
- Stress
What are the common risk factors?
Smoking is strongly linked to increased risk of HS and more severe symptoms. Family history and obesity are also risk factors. Other health conditions linked to HS include:9,11,12
- Metabolic syndrome – This includes high blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels. Together, they increase the risk of heart disease, stroke, and type 2 diabetes.
- Thyroid disease
- Joint disease
- Inflammatory skin conditions
- Axial spondyloarthritis – This inflammatory condition leads to arthritis in the spine and pelvic joints
- Inflammatory bowel disease
- Polycystic ovary syndrome – This hormonal disorder may cause cysts on the ovaries
- Squamous cell carcinoma – a common form of skin cancer
How is HS diagnosed?
When the first symptoms of HS appear, most people usually see a primary care doctor. Because HS is not very common, many doctors may not recognize it at first. There is no test to identify the disease. Getting the right diagnosis may take up to 7 years.6,9
A dermatologist, a doctor specializing in the skin, diagnoses HS by:6
- How the lesions look
- Typical locations of the lesions
- How often flares occur
- Age when symptoms began
- Poor response to antibiotics
- Lack of infection that affects the whole body
A doctor may also test a sample of the skin or discharge coming from any sores.
How does it affect you?
The pain, odor, pus, and appearance of HS often impact the social lives, employment opportunities, and emotional well-being of people living with the condition. Effects include:13-15
- Embarrassment, social isolation, and sexual dysfunction
- Loss of workdays and productivity. These factors, in turn, may reduce chances for career advancement.
- Depression and anxiety
How is it treated?
There is no cure for HS, nor is there one best treatment option. Instead, treatment depends on the person. Treatments usually include several methods to reduce symptoms, relieve pain, and heal wounds. They may include:2,11,16
- Local medicines applied on the surface of the skin or injected into the lesions
- Systemic medications that work throughout the body
Surgery - Negative pressure therapy to help wounds heal faster by increasing blood flow to the wounds, removing excess fluids, and preventing infections
- Diet
- Home remedies
- Lifestyle changes, including stopping smoking, losing weight, and reducing stress
- Complementary and alternative medicine
HS itself is rarely life-threatening, but it does increase a person’s risk for heart disease and suicide. If you have HS, your doctor may refer you to other specialists to help reduce risks and improve your quality of life.2,12